Coronavirus In Colorado: Hospitals Plan For Surge Of Patients, Shuffling Of Supplies
(CBS4) - Despite a conflict between the federal government and the state of Colorado over badly-needed medical equipment during the coronavirus pandemic, the state's hospitals appear to be ready to share supplies between facilities. Hospital officials don't expect facilities will attempt to out-maneuver one another for resources like has happened at the government level. But if the rate of spread of the COVID-19 virus ramps up and hospitals fill up, those plans could change.
"The next two weeks will be telling," said Julie Lonborg, Senior Vice President of Colorado Hospital Association, told CBS4. "If we continue to see the volume of patients coming in that we have in the last weeks, we will be challenged to keep up with space, supplies, and staff. Hospitals have added capacity, but we really need to flatten the curve as well.
"If we manage to flatten the curve, we hope to be OK."
Flattening the curve, she admits, is directly connected to people respected the advice of health departments and the governor's stay-at-home order.
"We know we can't expand capacity enough," Lonborg said, "if people don't stay at home."
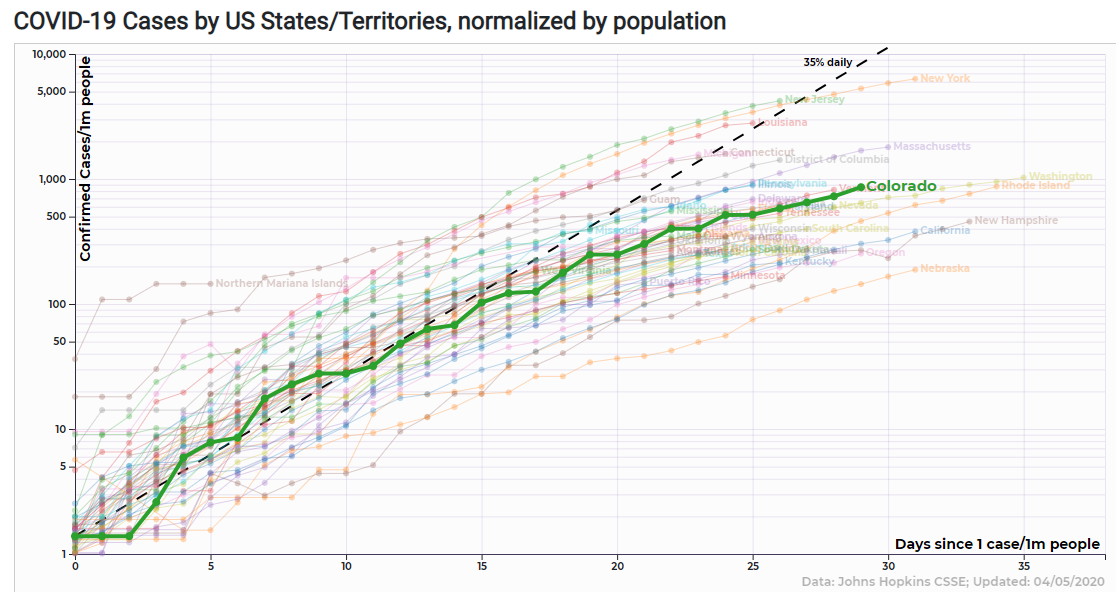
Colorado's prospects are mixed. Some data shows Colorado's cases on a steady, predictable climb. However, Dr. Deborah Birx, coordinator of the White House's coronavirus task force, said last week that Colorado is among those states on the verge of an upswing in mortalities.
As well, Gov. Jared Polis's request last Thursday to Vice President Mike Pence for supplies was unmistakably urgent.
"We are facing a crisis-level shortage of these essential supplies to protect our health care workers and first responders," he wrote. "Colorado's COVID-19 death rate is rising faster than any other state right now."
Friday night, Polis went on CNN to say Colorado's order for 500 ventilators and other supplies had been canceled by the manufacturer - because the items were being bought by the Federal Emergency Management Agency.
"Either be in or out," Polis told CNN's Don Lemon. "We can't compete against our own federal government, so either work with us, or don't do anything at all. But this middle ground where they're buying stuff out from under us and not telling us what we're going to get, that's really challenging to manage our hospital surge and our safety of our health care workers in that kind of environment."
"Really disappointed," Lonborg reacted. "It would be wonderful if we had great coordination at the federal level. That's frustrating."
The Associated Press reported Saturday other problems in private sector, too, where some physicians were reporting N95 masks which normally sell for less than a dollar were marked up to $10 a piece.
But Lonborg said pricing of equipment and supplies is not as much an issue for Colorado's hospitals as access.
"What's more concerning is if we can't get them," she said.
That is not a problem at this point for the UCHealth hospitals, according to spokesperson Paula Freund.
"While we have seen some exorbitant prices being quoted for masks," Freund said, "we have not had to pay those prices. Our supply chain has contracts with many national suppliers, and we continue to get shipments of the supplies we need. At this time, we have adequate inventories of PPE (personal protective equipment) including masks, gloves, etc., and all of our staff and providers have the equipment they need to stay safe and to provide safe care for our patients."
Lonborg predicted no competition would develop between Colorado's hospitals for resources, if the number of cases remains manageable.
RELATED Rural Colorado Hospital Receives Much-Needed PPE
"I will counter that it will set off a chain of cooperation like we've never seen," she said. "We know how to do this in Colorado. We know how to do this across the nation. We talk."
A new discussion is taking place this week, Lonborg added. Until recently, hospital staff did not foresee a potential shortage in certain sedatives and pain relievers.
"A week ago we weren't talking about medications," she said.
Sunday, state agencies enacted protocols for hospitals in the event that the number of critical care patients exceeds the number of ICU (intensive care unit) beds. Hospitals were instructed with specific staffing for triage teams. Those teams were given rigid requirements for the considerations they should weigh - future availability of life-saving supplies, severity of illness, likelihood of survival - when making life-or-death decisions about patients. Also mandated was what those teams should not consider - ethnicity, immigration status, gender identity, and criminal history, among others.
Currently, Lonborg said, hospitals are learning that the most ill COVID-19 patients are requiring much longer stays on ventilators and in hospitals than doctors had expected. That is a troubling fact as hospital staff eye a possible increase in the number of incoming patients. Possibly many more.
"Hopefully there will be enough time between spikes in the bigger cities that equipment and supplies can be deployed," she said. "Right now we're just trying to keep everyone who is working (in hospitals) healthy. That is an uphill battle."




