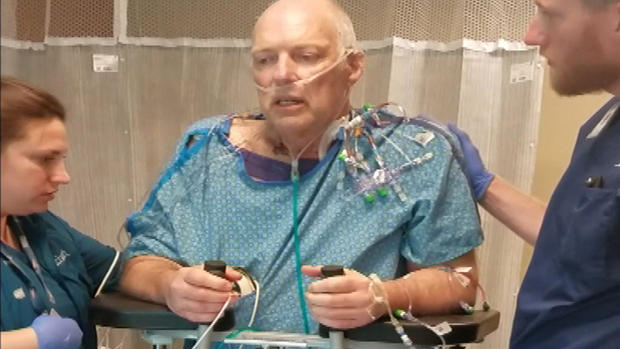
'The Day I Died': Dr. Dave Hnida Shares His Story
(CBS4) -If you had told me I was going to have a heart attack someday, I would have thought you were kinda crazy. If you had told me I was going to have a heart attack that day, I would have thought you were really crazy.
A snapshot of June 2, 2019, shows a 64-year-old guy in really good health, physically active, healthy eater, normal weight, and blood pressure and cholesterol numbers that made my doctor happy. A cardiologist who had performed a stress test and cardiac scan three years before told I had the heart of a 40-45-year-old. I thought I was living the golden life. Well, that golden life almost screeched to an abrupt end that 2nd day of June, and I didn't even recognize I was on the road to dying.
The day was a pretty normal Saturday. Went for a hike. Moved some furniture. Watched some baseball.
Took down some bicycles from the garage hooks to tune up the brakes. Bicycles that would wind up lying on the floor of the garage surrounded by dust gathering tools for the next three months.
That night I woke up at about 4:30 a.m. with what I thought was a "crick" in my neck, and a little muscle tightness below in my upper back. When shifting around didn't help, I hopped out of bed and did some stretches and cursed those bikes I had pulled down from the garage ceiling hooks. I went back to bed, but just couldn't get comfortable -- still it wasn't pain that even deserved a Tylenol. My "pain scale" was maybe a 1 of 10… 2 of 10 if I wanted to complain. It was all just so weird.
Did I think heart attack? Nah. Aortic aneurysm? Runs in my family. Blood clot in my lungs? No shortness of breath. In fact, I had no nausea, sweats, chest discomfort or anything else typical of serious things. Actually, I felt good! And to add another layer of insurance, I trotted up and down the basement stairs a few times. No change.
At 6:30 a.m. I started with a funky little cough. Still had that muscle weirdness in my upper back and base of the neck, as well.
I went back upstairs and decided to wake my wife and head to the ER in Littleton. Something just wasn't right. Probably a waste of time, but better to play it safe.
When we got there, I jumped out of the car and walked into the hospital, uttering the moronic words to the receptionist, "I really don't think I need to be here but I've got this weird pain in my neck and back."
The next thing I know I'm in a wheelchair, being speed-pushed into an exam room, and hooked up to oxygen, monitors, and IV lines. Just like I've done thousands of times over the decades to my patients who had classic or not-so-classic heart attack symptoms.
I remember the ER doc reading the EKG, shaking his heading slightly, and saying, "Well Dave, for guy who looks pretty good, you're having a massive anterior wall STEMI." Doctor-talk for a major heart attack. My jaw hurt from the force of it dropping like a boulder.
The next step was a trip to the Cath lab, where a different doctor threaded a catheter from my arm to my heart, injected some dye, and announced, "Man, you've got a complete blood blockage of your LAD. You need to stent to open that fellow up." I'm lying there thinking LAD -- Left Anterior Descending coronary artery. The so-called "widow-maker" The blockage with the highest percentage of death.
Crap.
I was having a massive heart attack and didn't know it. I should have, but I didn't.
He put in a stent to get the blood flowing again, but I felt no change. He then told me my heart wasn't pumping so well, so maybe they could put in some little gizmos to help strengthen the heart function.
Of course, do anything you need to.
And then, just like a sentence in a novel when a guy gets clubbed in the back of the head -- the world went black.
I barely remember anything that happened over the next 36 hours, but was later told my kids rushed to the hospital, including one who endured a worry filled three-hour flight across the unknown to get to Denver. Other family came. Friends came. My priest came. And they told me that first day, I wasn't too bad, even talking a little and smiling.
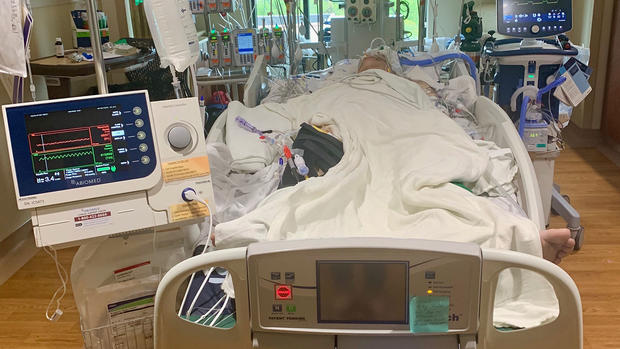
Fortunately, none of them were in the room the next day when the buzzers and alarms went off, and the overhead speakers blurted out "Code Blue. Code Blue. ICU." I had three cardiac arrests and was shocked back to life each time. My heart was just a piece of worthless meat that was worsening by the hour, and there was little that seemed to slow down that decent into the final crevasse. I had tanked.
Cardiac arrest number four struck a little later, and I wonder to this day whether it was a true near-death experience. I made the journey back to Christmas as a kid, making a game-winning basket in high school, pitching a solid game against Princeton in college, my marriage, the births of my children. It all was good stuff. No bright lights. No eternal darkness. Just good stuff.
Then lightning struck. This time I felt the shock, and I can't even describe what a zillion volts from paddles feel like, but it sucked. I even remember saying, "What are you doing to me!"
Maybe a miraculous turning point had been met, but it wasn't in the cards.
I continued to slide. The staff called my family in from the waiting area and it was gently suggested that each say a goodbye.
In the meantime, a friend and colleague, Dr. Ryan Jordan, was working the phones, and eventually got a thumbs-up for a transfer. The University of Colorado Hospital said they'd be willing to try to come up with some different approach. Last ditch. Poor odds. It would be a miracle if I saw morning. I just needed to get there.
And that's how I took my first helicopter ride since I was a doctor in Iraq.
Next Blog: What Becomes Of A Broken Heart?