'What Becomes Of The Broken Hearted?' Dr. Dave Hnida Describes His Heart Transplant
(CBS4) - It was a helicopter ride I will never forget, or remember. After a massive heart attack and several cardiac arrests in June, my heart was barely pumping any blood, and without some extraordinary measures, I would die.
In Denver, one of the places that offered a thin ray of hope was the University of Colorado Hospital. Doctors there believed the answer was a heart transplant ... but I needed to be kept alive until I could get one, and they had a machine that might be able to do that.
An ambulance to get me the 24 miles from one hospital to the next was out of the question. But a medical helicopter could fly above the Mile High City to get me there in minutes. My family followed behind by car, hoping that I'd be alive when they arrived. Their drive seemed agonizingly slow; I was unconscious during my journey, and would be so for the next two days.
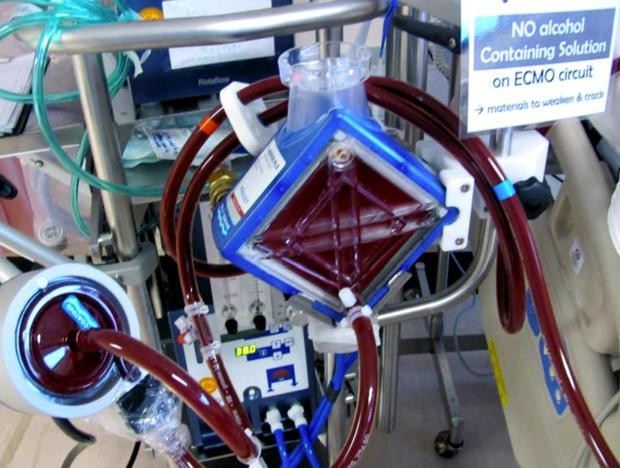
I went straight from the landing pad to surgery, where doctors hooked me up to a machine called ECMO, or ExtraCorporeal Membrane Oxygenation. As a physician, I had heard of it, but knew next to nothing about it.
It's basically a portable heart-lung machine, with a myriad of tubes like garden hoses running in and out of a variety of blood vessels. The blood comes out, gets cleaned, replenished with oxygen, then pumped back into the body.
It worked, or at least kept me ticking. My family was told the outlook was still grim, but the staff thought I had a fighting shot. Hopefully the ECMO would do the work of my failed heart, allowing it, and the rest of my organs to have a little recovery time.
I finally woke up, saw my family, and quickly realized I was a prisoner to a million and one tubes running from my body to some machine next to the bed. I couldn't move. Then again, I was so weak, I couldn't even raise my arm inches off the bed.
Now all I needed to do was wait for that transplant. But then came a major glitch. The shock of the heart attack and cardiac arrests caused my kidneys to shut down. And kidney failure makes you ineligible for a new heart.
I was taken off of the transplant waiting list, and would be off for close to two weeks as we all waited for the kidneys to come back to life. Slowly and gradually they did. But the clock was ticking rapidly; you can't stay on ECMO forever. For most, the average time on the machine is several days ... I was going on my third week. And the longer you're hooked up, the higher the risk of complications and death- a point driven home when one night when the machine unexpectedly clogged, and left me gasping for air and turning blue. Before I died again, the machine, and me, were fixed by about 15 people who sprinted into my room.
The third week of June, I was back on the waiting list, and less than 24 hours later, one of my doctors came into the room and said "You're not going to believe it, but we think we have a new heart. If you want it."
I had to decide immediately. Of course I wanted it, then immediately thought, geez, someone had died somewhere. And this person had a family, who was certainly grieving. Then I thought of my family, who I had put through hell. It was a no-brainer.
I learned the factors that go into who gets a transplant, which explained a lot about why I was at the top of the list:
Level of need. I would die soon without a transplant.
Compatibility. There needed to be a match of blood type and other immune factors.
Location. The donor heart needs to be fairly close to the recipient. You've got about 4-6 hours to get the new heart in or else it may not be viable.
Size. The donor heart needs to be a good fit for the patient's chest. It can't be too small or too big. I' 6-foot-3 and 215 pounds, so the donor had to be a fairly good sized person.
Besides that, we were not told anything specific. No name, location, circumstances, or any information which would violate the donor's and his/her family's privacy. It would be six months before I would be allowed to write an anonymous, unsigned letter of thanks, should they choose to accept it.
Once I made the decision, time sped up, but at the same time crawled. A lot was going on behind the scenes, such as taking other organs from the donor, such a lungs, kidneys and liver. It gave me a lot of time to think.
Was I afraid of surgery? Not really. I had already been through a lot, and knew how a transplant worked. And frankly, it would be easy on me since I'd be fast asleep. I felt bad for my surgeons, it was nearly 10 p.m.
The new heart had been inspected and tested to make sure it was suitable. Then it would be flown to Denver.
In the meantime, I would be in OR during its journey. A surgeon would make a 10-inch incision in my chest, then use an oscillating saw to cut my breastbone in half. I would then be cracked open like a walnut with a rib spreader. (I actually knew how to do this from my war experiences).
The big blood vessels to and from the heart would be tied and clamped off, cut, and I would be attached to a heart/lung machine.
My own heart would not be cut out and removed from my chest only after the new heart arrived on-site and inspected.
The new heart would then be sewn in, and hopefully it would start beating after being on ice for several hours. Warm blood would gradually begin to flow through the new heart, surgeons would look for micro-leaks, and, if necessary, hit me with mini-paddles to shock the new heart into beating again. The breast bone is then wired back together again.
The whole procedure took close to six hours.
I woke up in my room, saw my family and did not see the ECMO tubes. I guess I made it.
Before drifting back off to sleep, I heard my nurse say, "Don't get too comfortable. Tomorrow, you're up and out of bed".
The beat goes on.
Watch For My Next Blog: Life On The Other End Of The Stethoscope