'The Heroin Fix': Supervised Injection Facilities Are Lifesavers For Those Who Use Them
By Mark Ackerman
VANCOUVER, BC (CBS4)- The City of Denver is exploring the idea of setting up supervised injection facilities, where drug addicts can safely shoot up, as a means to prevent drug overdoses.
The idea is modeled after an existing program in Vancouver, Canada, which has the highest concentration of injection drug users in the world, according to health officials there.
CBS4 Investigator Brian Maass traveled to Vancouver to see firsthand how the injection centers are impacting Vancouver's opioid problem.
Last year, more than 1,000 people in Vancouver overdosed and died. This year, Vancouver is on pace to surpass that death total.
Dr. Mark Lysyshyn, Medical Officer at Vancouver Coastal Health, says Vancouver is in the midst of a "public health crisis" calling the overdose deaths "a provincial emergency."
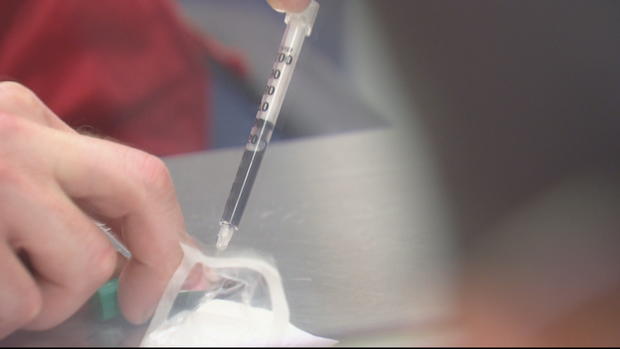
In an effort to prevent overdose deaths, the government has established safe injection sites where addicts bring their own drugs and receive clean needles and other supplies needed to shoot up. They inject under the watchful eye of medical professionals standing by ready to reverse an overdose.
Vancouver's first supervised injection facility, Insite, was established in 2003. Roughly, 600 people use the facility to inject drugs every day.
"No one has ever died from an overdose there," said Dr. Lyshysyn who said medical professionals at Insite successfully reverse 10 to 20 overdoses per week.
Just blocks away from Insite, CBS4 visited a new supervised injection site called The Powell Street Getaway, run by Keir McDonald, an Australian lawyer, who recently moved to Vancouver to help in the fight against heroin.
Maass asked McDonald a basic question: "Some people might find it shocking that the government funds a facility like this?"
"What has been shocking is losing 1,000 lives last year even through the work we are doing," McDonald replied. "Shocking is not doing anything."
Soon, drug users would fill the five metal stalls injecting and inhaling a variety of drugs, as CBS4 cameras recorded the accepted drug use.
Shane and Kayla were the first inside, declining a nurse's offer to test the contents of the drugs they brought. They gathered clean supplies, cooked the drugs with a lighter and injected drugs into their arms.
"I was working and everything was good," said Kayla, "I started doing it and everything got out of control."
Now she says she shoots up 12 to 15 times a day depending on how much money the couple can make doing odd jobs and selling drugs. She says she's overdosed 10 times and actually seeks the much stronger and cheaper narcotic fentanyl, saying she "likes it better than heroin."
"I don't want to die," Kayla said. She came to the supervised injection site because she had previously overdosed in an alley where "sometimes people don't get found."
Shane said he prefers the injection centers saying they are "clean, safe and not sketchy, like in an alley."
He and Kayla are making a plan to get clean and leave Vancouver's lower east side where they were living in a shelter.
Guy Felicella credits supervised injection sites for helping him turn his life around.
"If the safe injection site didn't exist," he said, "It's a no-brainer, I wouldn't exist either."
Felicella was a heroin addict for two decades who shot up in Vancouver alleys as often as 30 times a day. He supported his habit by selling drugs and armed robbery, eventually using heroin in a safe injection facility where he overdosed six times. All six times the medical staff brought him back to life.
"Is this the solution? No," he said. "But, it's part of the solution that needs to be included."
The supervised injection facilities were a resource that kept him alive until he was ready to change. Then, the facility connected him with treatment.
"You can't save a dead addict," he said.
Now Guy is clean, has a wife and two children and works at an addiction clinic.
But, even with safe injection facilities dotting Vancouver's lower east side, many addicts are uninterested in changing their patterns.
CBS4 visited a place nicknamed "death alley" where a constant stream of addicts shoot up, nod off and use heroin, one after another.
"It's extremely emotional," said Sue Oulette who helps addicts who overdose there. "This week three people I know are gone."
A man named Matthew told CBS4 he shoots up half a dozen times a day, but chooses not to use a safe injection facility.
"They hang over you," he said. "Too many rules."
Matthew said he had shot up two minutes before speaking to CBS4.
In the short time CBS4 was in that alley, an ambulance took away a woman who had overdosed. Yet, addicts continued to inject, right in front of paramedics, police and CBS4 cameras.
In Vancouver, heroin addiction is viewed more as a healthcare or medical problem, and not a criminal justice issue. The common thinking among healthcare professionals and anti-drug activists in Vancouver is that you can't arrest your way out of the heroin epidemic; other avenues need to be considered.
Lyshysyn said supervised injection has led to "less crime, less public injection" and "fewer discarded needles" which he says are "all benefits to society."
But, even as Maass was interviewing Lyshysyn in the alley behind his home, people were injecting only a few feet away, oblivious to the camera or simply unconcerned about the presence of a media crew.
"We are talking to you in this alley and there are people shooting up heroin right next to us one right after another," said Maass. "How well is the program working if people are still sitting in alleys and shooting up heroin?"
"This is the neighborhood I live in. This is the problem we are facing," Lyshysyn said. "We haven't been able to solve this problem."
But, he said supervised injection sites are part of the solution, along with law enforcement, prevention and treatment. With drugs getting stronger and cheaper, Lysyshn says American cities need to move towards supervised injection facilities, and fast.
"If Denver isn't seeing this problem it is going to see it soon," he said. "If it doesn't have facilities like this it isn't going to be prepared."
Mark Ackerman is a Special Projects Producer at CBS4. Follow him on Twitter @ackermanmark